Living with sudden urges to pass urine or frequent trips to the toilet can be frustrating and disruptive. Overactive bladder, often shortened to OAB, affects daily routines, sleep, and confidence for many adults. Although it’s a common bladder condition, it’s often misunderstood or dismissed as a normal part of ageing.
Stay with us until the end to understand what an overactive bladder is, why it happens, and how it may be managed with the right support.
What Is an Overactive Bladder?
Overactive bladder describes a group of urinary symptoms, not just a single disease. The main feature is a sudden and strong need to urinate that’s hard to delay. This urgency may happen with or without leakage, which some people find distressing.
Common signs include needing to urinate more often than usual, waking at night to pass urine, and feeling unable to fully control bladder urges.
Possible Causes and Risk Factors
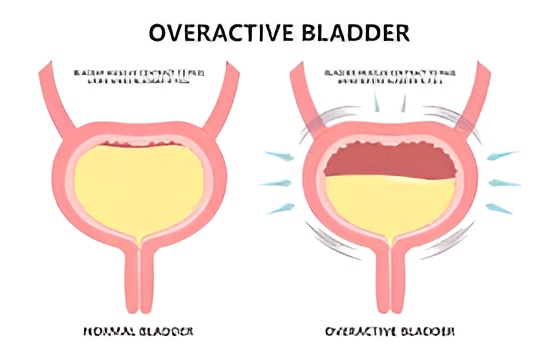
The bladder works by storing urine and releasing it at the right time. With overactive bladder, the bladder muscle may contract too early, even when it isn’t full. This change might be linked to nerve signals between the bladder and brain.
Several factors may increase risk. These include ageing, certain neurological conditions, bladder irritation, or previous pelvic surgery. In some cases, no clear cause is found. Importantly, overactive bladder isn’t the same as a urinary tract infection, although symptoms can feel similar.
How Overactive Bladder Is Assessed
Assessment usually starts with a detailed discussion about symptoms, fluid intake, and lifestyle habits. Simple tests, such as urine checks, may help rule out infection or blood in the urine.
Specialist evaluation may be helpful when symptoms persist or affect quality of life. At a reputable London urology clinic, investigations like bladder scans or cystoscopy might be considered to understand how the bladder is functioning and to exclude other conditions. This step helps ensure symptoms are treated appropriately.
Non-Surgical Treatment Options
Many people notice improvement through practical lifestyle changes. Reducing caffeine, spacing fluid intake, and bladder training exercises may help improve bladder control over time. Pelvic floor exercises are often recommended, as stronger muscles may support better bladder function.
Medication may also be discussed. These medicines aim to relax the bladder muscle, which may reduce urgency and frequency. Effects vary between individuals, and side effects are reviewed carefully before continuing treatment.
When Further Treatments May Be Considered
If symptoms continue despite first-line options, other treatments might be explored. These may include targeted therapies delivered directly to the bladder or nerve-based treatments that help regulate bladder signals. Decisions are usually guided by symptom severity, overall health, and personal preferences.
It’s important that any treatment plan is reviewed regularly, as bladder symptoms can change over time.
Supporting Long-Term Bladder Health
Managing overactive bladder often involves patience and ongoing support. Keeping a bladder diary, attending follow-up appointments, and discussing concerns openly may lead to better outcomes. Many people find reassurance in knowing that symptoms are common and manageable with the right care.
Final Thoughts
Overactive bladder can feel isolating, but it’s a recognised medical condition with several effective ways to manage symptoms. Anyone experiencing persistent bladder changes should seek professional advice rather than self-managing in silence.
Always consult a qualified healthcare professional before making decisions about bladder or prostate treatments and medications.